The pandemic is far from over. At the end of 2021, only five African countries (Cabo Verde, Mauritius, Morocco, Seychelles, and Tunisia), less than 10% of Africa’s 54 nations, were projected to hit the target of fully vaccinating 40% of their population. In the absence of wide scale vaccine rollouts, the continent must continue to rely on the tried and tested non-pharmaceutical interventions that have proved impactful in managing the outbreak until this point.
Some of those lessons learnt are highlighted in new reports from the African Health Observatory Platform on Health Systems and Policies (AHOP). Five National Centres from AHOP, based in Ethiopia, Kenya, Nigeria, Rwanda, and Senegal, reflected on country policies to both contain the outbreak and coordinate responses during the initial phases of the pandemic. Policy interventions and the government structures that emerged were tracked and set alongside their potential health impacts. What emerged was a picture that was common across many African states — namely a broad set of challenges associated with introducing a range of public health measures and with coordinating implementation across sectors and stakeholders.
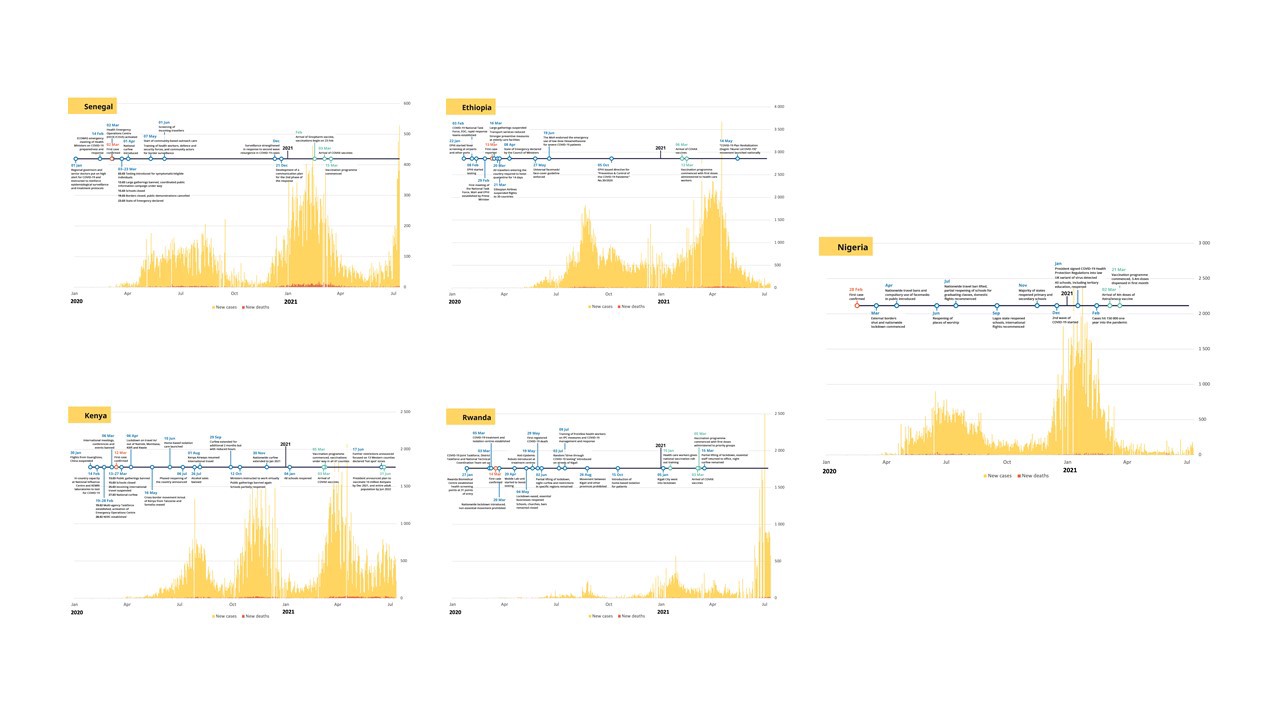
Since the start of the pandemic, more localized concepts of containment have been favoured reflecting the need to balance stringent prevention of transmission with the need to sustain livelihoods. In Ethiopia public adherence to preventative measures was high. The population quickly adopted respiratory hygiene measures, such as face coverings. Adherence remained high with 90% of public transport drivers still adhering eight weeks after their introduction.
Across the region, early implementation of subnational travel limits alongside cross-border travel bans, were linked into continent-wide efforts to limit movements. Thus, contributing substantially to successful early containment of the first wave of the pandemic.
Within countries, multisectoral and multistakeholder responses were a common feature of the pandemic response. Kenya adopted a “whole of government” approach while Nigeria prioritised a multisectoral response looking beyond the Ministry of Health. This offered opportunities in the form of greater flexibility, inclusivity, and reach. However, such far reaching efforts presented challenges such as duplication of activities and disconnect between stakeholders, be it from national to subnational level, or between public and private efforts.
While vaccination is moving slowly because of the low number of doses dedicated to Africa, the continent must continue to advance and implement the basic public health tools at its disposal, including rapid antigen test scale-up; enhanced community work; surveillance activities for early case identification; contact tracing and facilitating referrals for testing and continuity of care. This also means continued government action despite significant gaps. Africa is facing multiple challenges of responding to the COVID-19 pandemic, among them, access to critical health resources like oxygen and vaccines. However, the continent is still the least affected by the pandemic (based on cases and deaths) compared to other regions. The next steps is to ensure that the continent prepares efficiently for future pandemics, using lessons from current challenges.
Where are we now?
Health response gaps were discussed at the 71st session of the WHO Regional Committee for Africa in August 2021. The adopted Framework for Strengthening the Use of Evidence, Information and Research for Decision Making in the African Region recalled that the African Region is still struggling to use health research evidence in health policies. Also noted was that countries in the Region routinely fail to produce locally relevant health evidence for policy formulation based on local needs and priorities.
Enabling policy makers to make decisions based on African realities, especially during a pandemic, is therefore of paramount importance. One of the responses to this need has been the establishment of the World Health Organisation’s Regional Officer for Africa’s COVID-19 Information Hub for Africa embedded in the integrated African health observatory.
This Hub has emerged as a necessity in the region as COVID-19 information is varied and diffused across several platforms and programmes. A direct consequence of this is the difficulty decision makers face in navigating multiple information sources. Through the COVID-19 Information Hub, policy makers can access all the information, reports, and latest news on COVID-19 in the African Region, in one centralized location.
For example, the epidemiological information page provides a real-time overview of the epidemiological situation across the 47 Member States of the WHO African Region and detailed information on the circulation of Covid’s variants. While immunisation remains a challenge in the African region, the dashboard provides a clear picture of vaccines administered and consequently quantifies immunisation needs in the region, as well as an overview of country and regional vaccination rates and available vaccines.
With all the uncertainty surrounding the pandemic, including the circulation of rumours and fake news, it can be challenging to have accurate information available. The public perception barometer available on the Information Hub serves as a tool to monitor public perceptions of COVID-19. The barometer is based on 3 areas: vaccines, case management, and non-pharmaceutical measures. In addition to gaining a better understanding of the population’s perceptions, the tool serves as a starting point for a deeper investigation to inform targeted decision making. Bringing together all the information on COVID-19 from across the various regional dashboards into one coherent and user-friendly platform, also acts as a comprehensive source of information for the public.
The Evidence Synthesis page features a multitude of knowledge products, namely published literature, best practices, policy briefs and guiding tools. These address topics such as the impact of COVID-19 on essential services, responses, interventions, the impact on other sectors and WHO management response.
Effective decision making based on relevant evidence will continue to be crucial as countries across the African region continue to respond to the pandemic. Actions up until now have often been despite the existence of health information gaps. Continued success and preparing for future health emergencies will need a restructuring of approaches to knowledge that allow rapid knowledge to be derived from available, accurate and real time information.